Abstract
Inactivating mutations in NF-kB pathway genes, such as the NF-kB inhibitor NFKBIE, are among the more frequent genetic lesions in chronic lymphocytic leukemia (CLL). However, the role of these genetic lesions in CLL pathogenesis and treatment resistance is still largely unknown and requires further study in in vivo models of the disease. To this end, we generated transplantable murine leukemias with inactivating NFKBIE mutations and investigated their impact on leukemia growth and response to ibrutinib (IBR) treatment. The NFKBIE mutations were introduced by CRISPR/Cas9 editing in two recently established autoreactive leukemia lines derived from the Eμ-TCL1 murine CLL model. These cell lines proliferate spontaneously in vitro in a BCR-dependent manner, but also respond with increased proliferation to certain microenvironmental signals, such as those generated by Toll-like receptor (TLR) stimulation (Chakraborty S et al, Blood 2021).
To investigate whether NFKBIE mutations can affect the proliferation of these cell lines in vitro, we performed competition experiments with mixed cultures of cells with wild type and mutated NFKBIE. Analysis of the clonal composition after 2 weeks showed no change in the mutant allele frequency (MAF), suggesting that NFKBIE mutations do not affect the spontaneous in vitro growth of the immortalized leukemia cells. However, repeated TLR or BCR stimulation of these cells with CpG-DNA, LPS, anti-IgM or autoantigen resulted in a 2-3 fold increase in MAF, suggesting that NFKBIE mutations provide a growth advantage when the cells are exposed to certain microenvironmental signals (n=3 experiments/condition, P<0.05 for each condition).
To investigate the impact of NFKBIE mutations on leukemia growth in vivo, the same cells were transplanted by intraperitoneal injection in wild type mouse recipients (n=8) and the clonal composition was determined 3 weeks later by MAF analysis of cells isolated from peritoneal cavity (PC), blood and spleen. A significant increase in MAF was observed only in leukemia cells isolated from the spleen (P<0.05), suggesting that microenvironmental signals that positively select NFKBIE-mutated cells are available only in certain tissue compartments.
Because mutations in other NF-kB pathway genes have been associated with resistance to IBR in mantle cell lymphoma, we next investigated whether NFKBIE mutations can also affect the response to IBR treatment. In vitro BrdU-incorporation experiments showed that IBR inhibits the proliferation of cells with mutated NFKBIE to a significantly lesser extent compared to cells with wild type NFKBIE (% proliferating cells with wild type and mutated NFKBIE, respectively, cultured without IBR: 90% vs 88%, P=n.s., with 0.2 μM IBR: 57% vs 73%, P<0.001, with 1.0 μM IBR: 28% vs 53%, P<0.001). Consistent with this finding, positive selection of NFKBIE-mutated cells was observed in the presence of IBR after 14 days in mixed culture competition experiments (mean MAF without IBR 47%, with 0.2 μM IBR 61%, p=0.032, with 1.0 μM IBR 64%, p=0.034). The greater resistance of NFKBIE-mutated cells to IBR was further validated by in vivo competition experiments showing a significantly greater increase in MAF in mice treated with IBR compared to controls in all three investigated compartments (n=4 mice/group, PC: P=0.029, blood P=0.029, spleen: P=0.001).
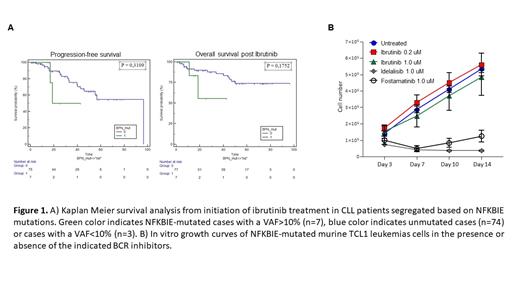
To validate these findings in the clinical setting, we investigated the presence of NFKBIE mutations in a cohort of 84 IBR-treated CLL patients. Mutations of NFKBIE were detected at pre-treatment in 10/84 patients, 7/10 with >10% VAF values. Kaplan Meier analysis showed a trend towards reduced progression-free and overall survival from the beginning of IBR treatment for NFKBIE-mutated cases (Figure 1A). Analysis of an extended cohort of over 200 cases is ongoing and will be presented at the meeting.
Finally, to investigate whether leukemic cells with mutated NFKBIE remain sensitive to other BCR inhibitors, we tested their growth in the presence of the PI3K inhibitor idelalisib or SYK inhibitor fostamatinib (Figure 1B). In contrast to IBR, both drugs inhibited the proliferation of NFKBIE-mutated cells in vitro, with a greater effect observed with idelalisib. Collectively, these data demonstrate that NFKBIE mutations can reduce the response to IBR treatment and suggest that such cases may benefit more from treatment with a PI3K inhibitor.
Marasca: Janssen: Honoraria, Other: Travel grants; AstraZeneca: Honoraria; AbbVie: Honoraria, Other: Travel grants. Tafuri: Roche: Research Funding; Novartis: Research Funding; Celgene: Research Funding. Laurenti: Janssen: Consultancy, Honoraria; AstraZeneca: Consultancy, Honoraria; AbbVie: Consultancy, Honoraria, Research Funding; Roche: Honoraria, Research Funding; Gilead: Honoraria; BeiGene: Honoraria. Gattei: abbVie: Research Funding; Janssen: Research Funding; Menarini: Research Funding.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal